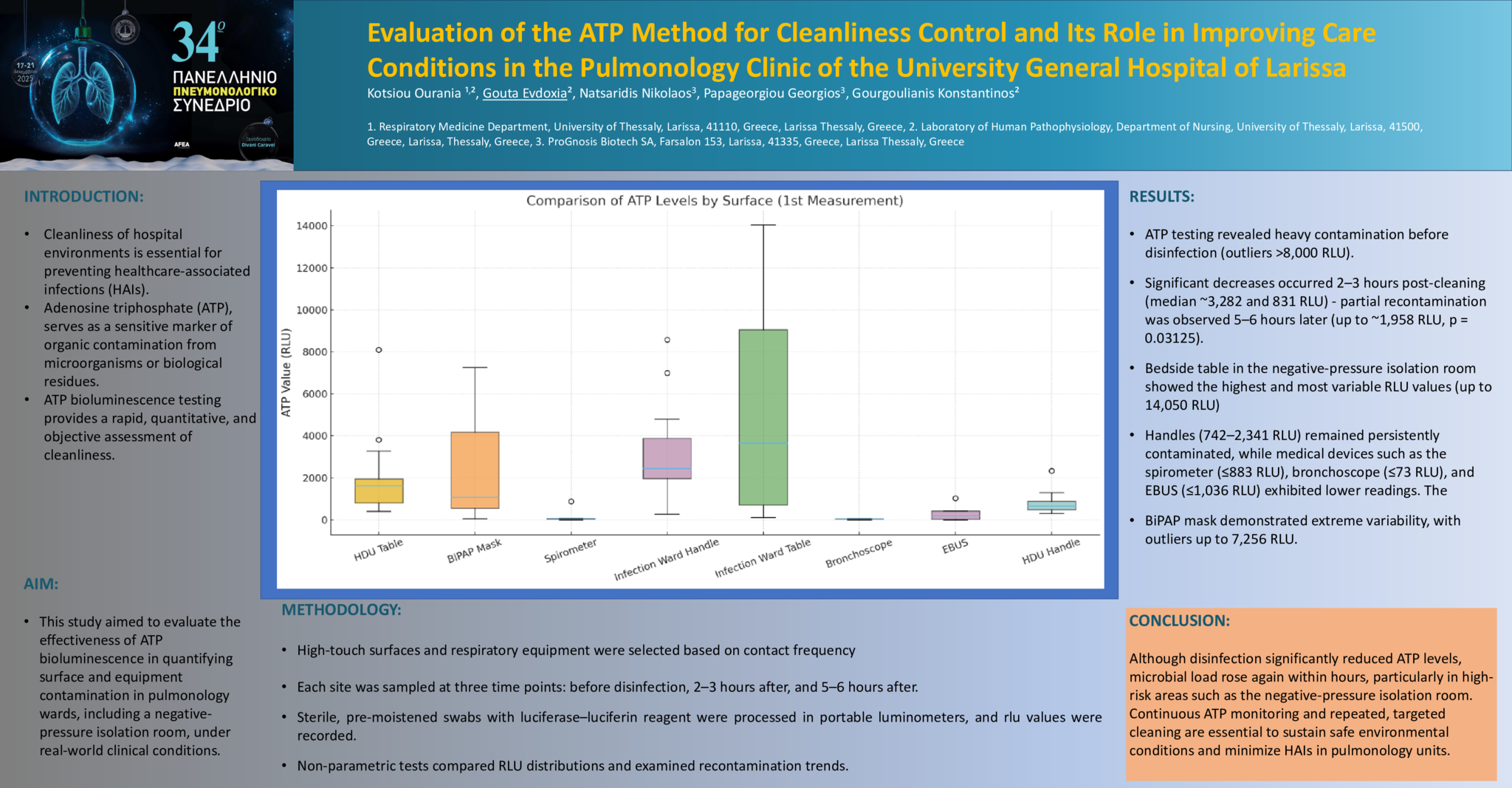
Background: Cleanliness of hospital environments is essential to preventing healthcare-associated infections (HAIs). Adenosine triphosphate (ATP), a universal biomolecule found in all living organisms, serves as an effective marker of organic contamination from microorganisms or residual biological material. ATP bioluminescence testing offers a rapid, quantitative, and objective assessment of cleanliness; however, it cannot differentiate pathogenic from non-pathogenic organisms or detect antimicrobial resistance. Objective: This study aimed to evaluate the effectiveness of ATP bioluminescence in quantifying surface and equipment contamination in pulmonology wards, including a negative-pressure isolation room, under real-world clinical conditions. Methods: High-touch surfaces and respiratory equipment were selected based on contact frequency and infection transmission risk. Each site was sampled at three time points: before disinfection (Measurement 1), 2–3 hours after (Measurement 2), and 5–6 hours after (Measurement 3). Sterile, pre-moistened swabs with luciferase–luciferin reagent were processed in portable luminometers, and Relative Light Unit (RLU) values were recorded. Statistical analysis using non-parametric tests compared RLU distributions and examined recontamination patterns. Results: ATP testing revealed heavy contamination before disinfection (outliers >8,000 RLU). Significant decreases occurred 2–3 hours post-cleaning (median ~3,282 and 831 RLU), yet partial recontamination was observed 5–6 hours later (up to ~1,958 RLU, p = 0.03125). The bedside table in the negative-pressure isolation room exhibited the highest and most variable RLU values (up to 14,050 RLU), confirming it as a critical surface for targeted intervention. Handles (742–2,341 RLU) also remained persistently contaminated, reflecting continuous hand contact. Medical devices such as the spirometer (≤883 RLU), bronchoscope (≤73 RLU), and EBUS (≤1,036 RLU) demonstrated lower readings but occasionally exceeded safety limits. The BiPAP mask showed extreme variability, with outliers up to 7,256 RLU, highlighting inconsistent disinfection. Conclusion: While disinfection significantly reduced ATP values, microbial load increased within hours, especially in high-risk zones such as the negative-pressure isolation room. Continuous ATP monitoring and repeated, targeted cleaning protocols are essential to maintain environmental safety and reduce HAIs in pulmonology units.
- 1 προβολή