Introduction
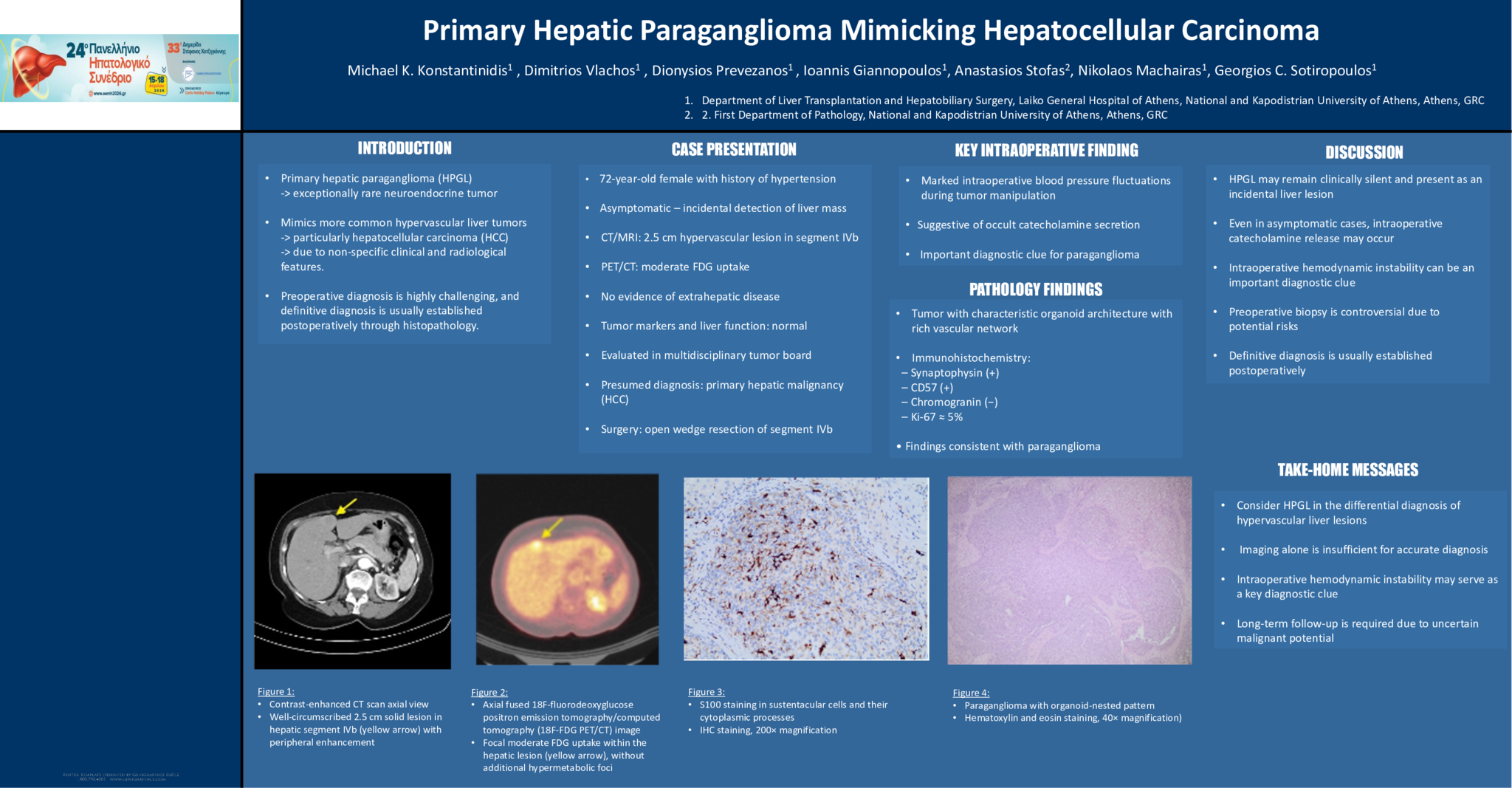
Primary hepatic paraganglioma (HPGL) is an exceptionally rare neuroendocrine tumor arising from sympathetic paraganglionic tissue within the liver. Although the liver is a common metastatic site for pheochromocytomas and paragangliomas, true primary hepatic involvement is extremely uncommon, with fewer than 20 cases reported in the literature. Due to nonspecific clinical presentation and radiologic characteristics, HPGL frequently mimics hepatocellular carcinoma (HCC) or other hypervascular liver tumors, making preoperative diagnosis challenging.
Purpose
To present a rare case of primary hepatic paraganglioma initially misdiagnosed as hepatocellular carcinoma and to highlight the diagnostic challenges, intraoperative findings, and management considerations associated with this entity.
Methods
A 72-year-old woman with a history of hypertension was referred to our hepatobiliary unit after incidental detection of a liver mass. Contrast-enhanced computed tomography (CT) and magnetic resonance imaging (MRI) demonstrated a 2.5-cm hypervascular lesion in segment IVb with peripheral enhancement. The patient underwent 18F-Fluorodeoxyglucose Positron Emission Tomography / Computed Tomography scan (18F-FDG PET/CT) which showed moderate uptake without evidence of extrahepatic disease. Laboratory evaluation, including liver function tests and tumor markers, was unremarkable. Based on imaging findings, hepatocellular carcinoma was suspected, and surgical resection was planned. The patient underwent open wedge resection. Histopathological and immunohistochemical analyses were performed. Postoperative Iodine-131 Metaiodobenzylguanidine (I-131 MIBG) scintigraphy was used to exclude extrahepatic disease.
Results
During tumor manipulation, marked intraoperative blood pressure fluctuations were observed, suggestive of catecholamine release. The postoperative course of the patient was uneventful. Histopathology revealed a well-circumscribed neoplasm with characteristic organoid architecture. Immunohistochemistry showed positivity for synaptophysin and CD57, focal S100 staining in sustentacular cells, and a low proliferative index (Ki-67 about 5%), consistent with paraganglioma. Chromogranin expression was negative. Surgical margins were free of disease. Postoperative I-131 MIBG scintigraphy demonstrated no additional lesions, confirming the diagnosis of primary hepatic paraganglioma. At six-month follow-up, the patient remains disease-free.
Conclusions
Primary hepatic paraganglioma is a rare and diagnostically challenging tumor that may closely mimic hepatocellular carcinoma on imaging. Intraoperative hemodynamic instability should raise suspicion for catecholamine-secreting tumors, even in clinically asymptomatic patients. Complete surgical resection is the treatment of choice and is associated with favorable short-term outcomes. Given the uncertain malignant potential of paragangliomas, long-term postoperative surveillance is essential.
- 8 προβολές